Your questions - our answers
DISCOGEL injection
How long must I stay in the hospital ?
Most often, it is about an ambulatory intervention: once arrived at the hospital; a light intervention is performed and the same day it is possible to go back home.
DISCOGEL: Mechanism of action
What is the mechanism of action ?
1 -Step of hernia decompression
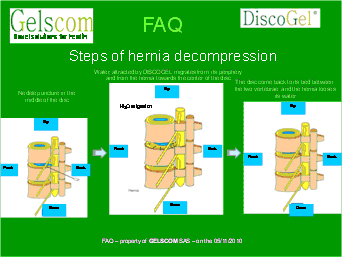
2 - Mechanism of action
- principally linked to the hydrophilic properties of the agent which make the gel soluble and who generates the migration of the water from the periphery of the disc (including hernia) towards his centre.
- The not soluble gel in the presence of water, precipitates and settles in the micro infractions of the disc to create so a «flexible soft prosthesis».
Note:
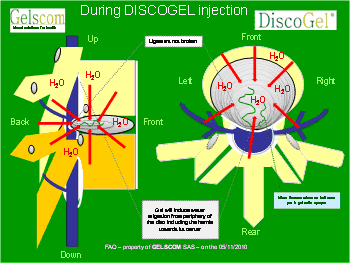
- At the time of injection, the radio opaque gel will find its way in the fissures of the disc to reach hernia (even if it is far from the point of injection of the disc)
- In the presence of water, the gel fills up hernia and fissures “highlighted” by radio-opaque compound included in the gel.
- The drainage of hernia contributes to fall the pressure of this one and on decreasing the stimulation of surroundings nerves (slipped disc decompression) then to speed up its necrosis and its disappearance.
- The disc becomes “waterproof” and the possible pro-inflammatory molecules remain sequestrated in the disc (and participate to break inflammatory process: therefore to diminish pain).
3-Herniated disc formation
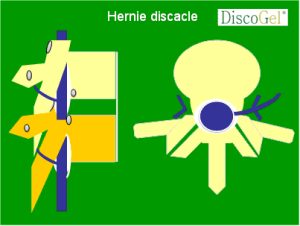
4 - During the injection of DISCOGEL
5 - the procedure
After the procedure
When can I expect recovery after DISCOGEL® intervention ?
A symptomatic improvement may occur between within 3 up to 6 weeks after the injection of DISCOGEL®. While in comparison with the conventional surgery well accomplished, 3 months are necessary.
What are results with DISCOGEL® ?
Accordingly to the publication: «Journal of Spinal Disorders and techniques » Oct. 2007 on and a percutaneous treatment of lumbar intervertebral hernias, the rate of results is considered very good or good for 91.4 % (group A: 202/221 patients). On patients with complicated hernias which were treated by DISCOGEL® (having a narrow channel, a foraminal hernia, a very painful hernia) belonging to the group B an automated percutaneous discectomy was additionally practiced. Patients of group C : DISCOGEL® was associated to a treatment by radio frequency. The hit rate in these two last considered groups as very good or good was respectively from 84 % and to 82 %.
What is the failure rate with DISCOGEL® who required subsequently a conventional surgery ?
According to the publication only 0.7 % (2/276 patients) requested a posterior surgery.
Does the treatment with DISCOGEL® forbid after an intervention by conventional surgical treatment ?
One of the advantages of DISCOGEL® is the conservation of anatomic bone and ligament structure of the rachis. So the option in a conventional surgery always remains opened.
What detachment is there on the treatment with DISCOGEL®, which is the Repetition rate ?
Over 5 years of monitoring, there were not repetitions.
Does the treatment induce an intervertebral disc collapse ?
This technique does not affect the height of the intervertebral space and the impact on the anatomy of the spine is conserved.
For what is the tungsten of use in DISCOGEL® ?
The tungsten is a radio opaque element (opaque to X-rays) used to show “in live” the gel under fluoroscopy to control the injection of jellified alcohol.
Ulterior radiological studies allow determining the site of the intervertebral disc injected and treated by DISCOGEL®.
How long is it possible to take back physical activities ?
The reintegration for physical activity (everything depends on type of exercise and individuals, but it is of almost of 3 up to 6 weeks (by comparison with 3 months for a satisfactory classical surgery without consequence).
After intervention on a cervical disc, is it necessary to carry a surgical collar ?
No, because it is necessary to re-develop muscles as much as possible the postural cervical muscles and to induce the resumption of muscular energy in the treated zone by watching not to force during the period of recovery.
As the region of the spine has tendency to generate sticking after a surgical operation, what procreates painful consequences. Does DISCOGEL® minimize this kind of risk ?
Yes, absolutely, because this intervention respects the integrity of the spine. Postural muscles around vertebras and are not injured. This minimizes risks of inducing collagen formation and sticking nervous endings of imprisonment which can radiate locally during movements.
How long DISCOGEL® last in the body?
DISCOGEL® is classified as an implant: it must remain in the disc permanently. To date, we have 7 years’ hindsight, so we can safely say at least 7 years.
Is there a risk of the product “bubble” moving?
Since the gel fills crevices and weakened areas to seal them, there can be no displacement of the gel, which remains sealed in situ. What’s more, the minimally invasive procedure leaves the anatomy of the area intact. It is not a conventional surgical procedure involving the cutting of tissue or postural muscles to gain access to the diseased disc. The anatomical architecture as such remains intact: the disc is retained in its natural position with no risk of migration. This is another distinguishing feature of this technique. There is no fibrogenesis following surgical sectioning.
Can tungsten leave the injection site via the bloodstream?
The tungsten is trapped in the network created by the gel, and forms a mass with it. Doctors have been using this compound to fill vessels in the brain for decades.
Note: As a reminder, this radio-opaque compound increases the user’s safety, as he or she can see the gel’s progress in the anfractuosities live on the image intensifier monitor during injection. The disc is a relatively isolated part of the body, which is why it cannot repair itself following a herniation, due to its very poor irrigation. The supply of nutrients and the elimination of toxins cannot bring about remission. As soon as a disc has become fragile, it can be said to have begun necrosis. The aim of the DISCOGEL® technique is to preserve the disc in the best possible condition.
How is DISCOGEL® absorbed and assimilated?
The network created by the cellulose derivative making up the gel cannot be assimilated by humans (we’re not ruminants!), so the flexible prosthesis ultimately formed by the gel + tungsten is not designed to be resorbed. As a reminder, the very poor irrigation of the disc makes it all the more difficult for the immune system to eliminate foreign bodies.
L'intervention
The procedure
DISCOGEL® preparation

The procedure
- The needle must be placed in the center of the disc.
- Injection time should be slow (5 min.) (it can be punctuated by stops so that the progress of the gel in the crevices can be observed on the monitor).
- The facet joints at the level of the hernia often suffer (inflammation) and cause pain -> for faster recovery this point should also be taken into consideration (injection of corticosteroids into the joints opposite the disc at the same time as injection of DISCOGEL® into the disc).
- Risk of DISCOGEL® leaking outside the disc? See publication: The Neuroradiology Journal 23: 249-252, 2010. A priori, this publication informs us that the damage that could be incurred, although improbable, is very low
If you cannot find an issue that concerns you, please go to page: Suggestion of non-treated questions ?